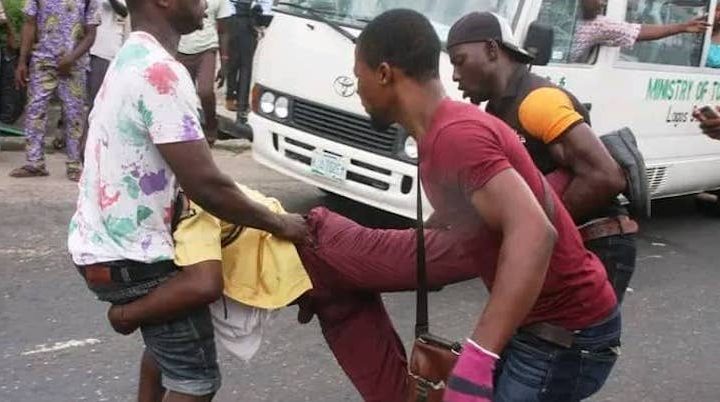Featured
Latest News

July 15, 2025
add comment
Governor Lucky Orimisan Aiyedatiwa of Ondo State has assigned portfolios to the 16 newly inaugurated commissioners, following...

July 15, 2025
add comment
Nollywood actress Angela Okorie has shared a worrying update about her health, revealing that fragments from the...

Actor Apologizes for Slapping Fellow Actor on Set
July 14, 2025
add comment

July 15, 2025
add comment
The Lagos State Governor, Babajide Sanwo-Olu, says attackers of the Lagos State Traffic Management Authority officers will...

July 14, 2025
add comment
Croatia captain, Luka Modric, has signed a one-year deal with AC Milan at the age of 39,...

July 15, 2025
add comment
Far-right Israeli Finance Minister Bezalel Smotrich says an attack on the Druze community in southern Syria proves...

June 28, 2025
add comment
The African Export-Import Bank has sealed a partnership deal with the Creative, Reality, Entertainment, Arts and Music...

July 15, 2025
add comment
Femi Adesina, former media aide to the late President Muhammadu Buhari, has defended his principal’s controversial medical...
July 12, 2025
add comment
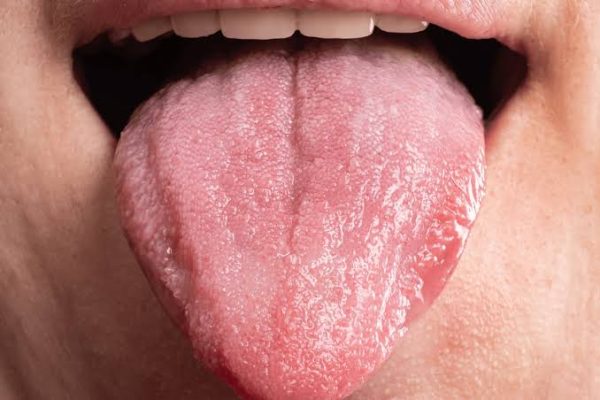
You can notice signs of HIV on the tongue during the early and late stages of the...

Probe Calabar hospital CMD Group Tells Tinubu
July 4, 2025
add comment

July 15, 2025
add comment
The University of Calabar has ordered over 300 students from its Dentistry Department to leave the institution...